Major Components of the Lymphatic System
|
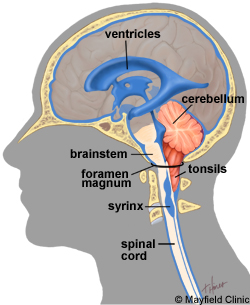
Tonsils
The tonsils are the first line of defense against infection in the body and can be located in many places around the ENT area, contrary to common belief. We actually have tonsils in our nose. Tonsils contain many pits called crypts which are used to trap bacteria and foreign cells and house many lymphocytes called T cells and B cells which help the tonsils produce antibodies to fight off these unwanted invaders. The antibodies secreted by the T and B cells stick to the targeted molecules trapped in the crypts in order to enlarge them so that they are too large to flow through the blood stream. This means they are forced into the lymphatic system where they can be safely drained out of the body. We have 5 tonsils within our nose and throat area; 2 lingual, 2 palatine and 1 pharyngeal. They help protect us from respiratory and digestive infections by trapping bacteria etc. before they can enter these systems. However there is some dispute over how effective tonsils are at preventing respiratory infection, particularly in adults. |
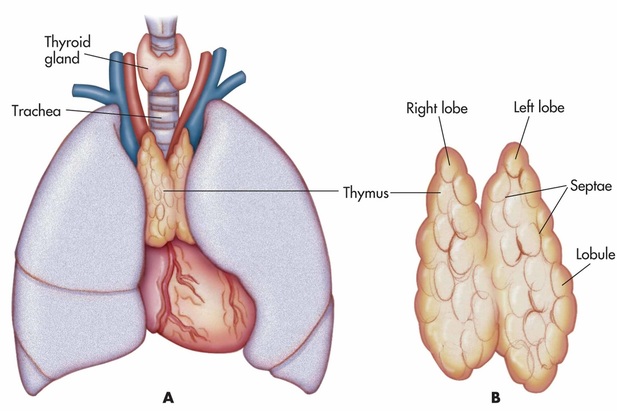
Thymus
The thymus is like the training ground for your T cells; and is slowly replaced by adipose tissue as the adaptive immune system develops. This process begins approximately as puberty finishes. T cells enter the thymus immature, where they are subjected to multiple hormones secreted inside the thymus and undergo rigorous testing and selection. All through our childhood, immature T cells are produced in red bone marrow and introduced to the section of the thymus called the cortex. Epithelial cells in the cortex of the thymus secrete harmful antigens for the immature T cells to "respond" to. The T cells which respond by destroying these antigens progress to the medulla of the thymus, the ones which do not are destroyed by macrophages which are also contained within the epithelium. This is called positive selection. Within the medulla, negative selection occurs. This is where the thymus secretes antigens which can be found within the body. For T cells to work effectively they must be able to distinguish between foreign cells and "friendly" cells, and for this reason, T cells which respond to antigens secreted in the medulla by destroying them will then commit cell suicide before they can leave the thymus and progress to the rest of the lymphatic system. This is a crucial process as it ensures the body doesn't produce lymphocytes that carry out specific responses on cells which are actually wanted. By the same token, selection in the thymus also produces T cells that will provide the best possible barriers of defense. This means only a very small fraction of the T cells which enter the cortex of the thymus then go on to be stored in subsequent parts of the lymphatic system. These cells can "remember" infections in order to provide specific response and activate the appropriate B cells to produce antibodies. Auto immune diseases can occur when the T cells have not matured properly within the thymus, which leads to inappropriate immune responses.
The thymus is like the training ground for your T cells; and is slowly replaced by adipose tissue as the adaptive immune system develops. This process begins approximately as puberty finishes. T cells enter the thymus immature, where they are subjected to multiple hormones secreted inside the thymus and undergo rigorous testing and selection. All through our childhood, immature T cells are produced in red bone marrow and introduced to the section of the thymus called the cortex. Epithelial cells in the cortex of the thymus secrete harmful antigens for the immature T cells to "respond" to. The T cells which respond by destroying these antigens progress to the medulla of the thymus, the ones which do not are destroyed by macrophages which are also contained within the epithelium. This is called positive selection. Within the medulla, negative selection occurs. This is where the thymus secretes antigens which can be found within the body. For T cells to work effectively they must be able to distinguish between foreign cells and "friendly" cells, and for this reason, T cells which respond to antigens secreted in the medulla by destroying them will then commit cell suicide before they can leave the thymus and progress to the rest of the lymphatic system. This is a crucial process as it ensures the body doesn't produce lymphocytes that carry out specific responses on cells which are actually wanted. By the same token, selection in the thymus also produces T cells that will provide the best possible barriers of defense. This means only a very small fraction of the T cells which enter the cortex of the thymus then go on to be stored in subsequent parts of the lymphatic system. These cells can "remember" infections in order to provide specific response and activate the appropriate B cells to produce antibodies. Auto immune diseases can occur when the T cells have not matured properly within the thymus, which leads to inappropriate immune responses.
|
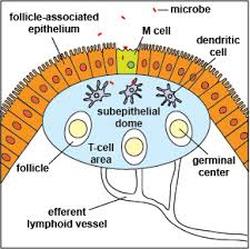
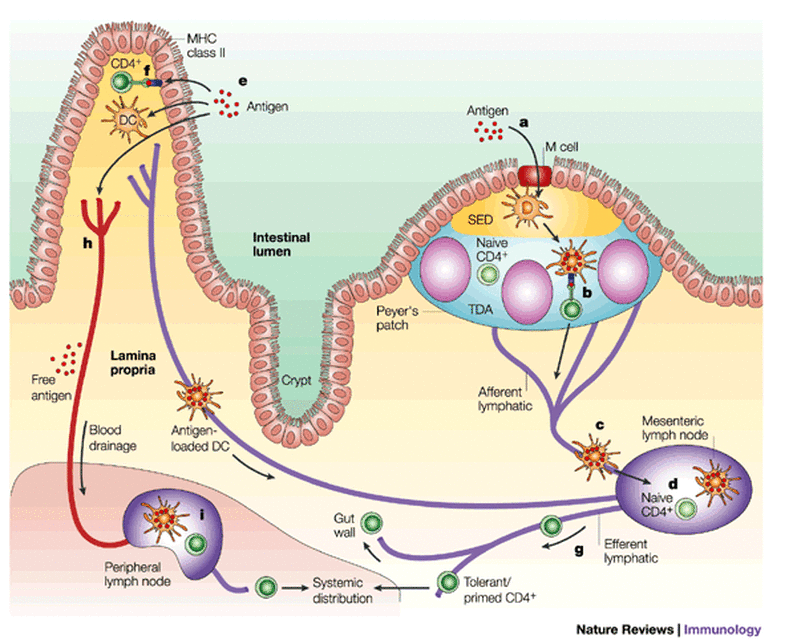
Peyer's Patches
Some of the epithelial cells which line peyer's patches are specialised to sample antigens in the intestine via endocytosis and send them to accessory cells (dendritic and T cells) located in the lumen. These are called M cells (or microfold cells) and are dispersed between the typical epithelial cells which line the intestinal tract. Any pathogens are then passed to the mesenteric lymph nodes where immune response is heightened to prevent further action on their behalf. |
|
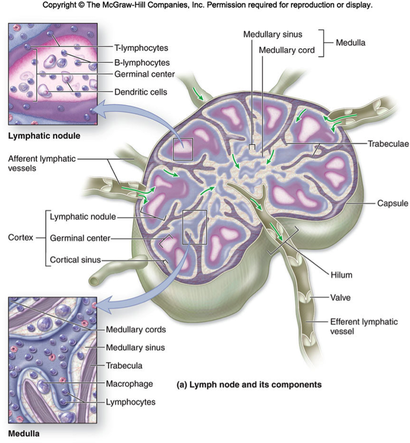
Lymph Nodes
Excess lymph which is collected in lymph vessels is transported to local lymph nodes where it can be properly filtered and introduced back into the cardiovascular system. Lymph nodes are encapsulated in a fibrous connective tissue matrix and filled with reticular connective tissue which is specialised to support lymphoid organs (reticular connective tissue is made up of type 3 collagen fibers). This tissue is branched in nature and works like a net to catch pathogens and allow the lymphocytes created in the germinal centre and macrophages located in the medulla to respond. During this filtration process dead cells, cancerous cells and cellular waste products are also extracted from the lymph. Efferent lymph vessels then transport the clean lymph fluid to lymphatic ducts to be secreted back into our blood. |
|
Spleen
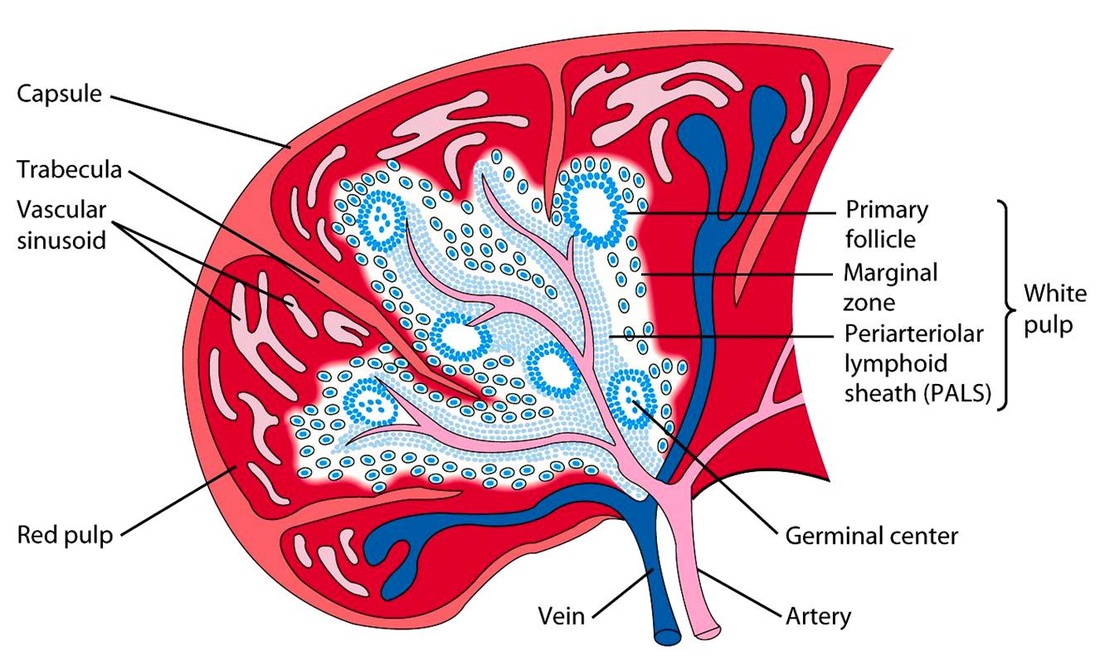
The spleen works in conjunction with lymph nodes to detect the presence of harmful microorganisms in the blood and induce the production of lymphocytes. It contains red and white pulp which act as storage matrix's for specific cells. Blood flowing into the spleen first encounters white pulp. The white pulp of the spleen holds the cells responsible for its immunological functions. T and B cells are stored within the white pulp of the spleen, which is where the blood is screened for pathogens. The T cells detect the pathogens, the B cells create the necessary antibodies to destroy them. The red pulp functions as a blood cell filter; macrophages within the spleen "eat" degenerate red blood cells (which may no longer be able to carry oxygen) and chemically extract the iron atoms from any haemoglobin molecules. The red pulp of the spleen is also a huge storage site for platelets. The spleen is not an essential organ in that it is not needed to sustain life; although it does provide a helping hand in the lymphatic system. |
Specific Immune Response
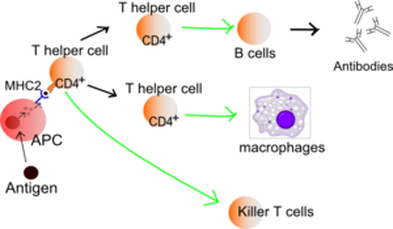
Humoural immune response is carried out by B cells (B-lymphocytes) which circulate the blood stream after maturation in the bone marrow or spleen. They remain in the blood until they sense a pathogen which presents the B cell's complementary antigens on its surface. When a few of these antigens bind with the B-cells this activates mitosis of the B-cells into plasma cell clones. These clones produce the appropriate antibodies to ward off the pathogens, and memory cells which archive the "specifics" of the infection in preparation for secondary response.
Cell-mediated Immune Response is carried out by T-lymphocytes which also circulate the body in blood. There are types of T-cell: killer cells, helper cells and suppressor cells. Killer cells break down pathogens and damaged and infected cells, helper cells trigger humoural response and suppressor cells control these processes by signalling when to stop i.e. cutting off production of antibodies. Certain pathogens are coated in antigens which fit receptor sites of selective T-cells; when the two meet and bind the T-cell divides into clones of its specialisation.
Cell-mediated Immune Response is carried out by T-lymphocytes which also circulate the body in blood. There are types of T-cell: killer cells, helper cells and suppressor cells. Killer cells break down pathogens and damaged and infected cells, helper cells trigger humoural response and suppressor cells control these processes by signalling when to stop i.e. cutting off production of antibodies. Certain pathogens are coated in antigens which fit receptor sites of selective T-cells; when the two meet and bind the T-cell divides into clones of its specialisation.
Non-specific Immune Response
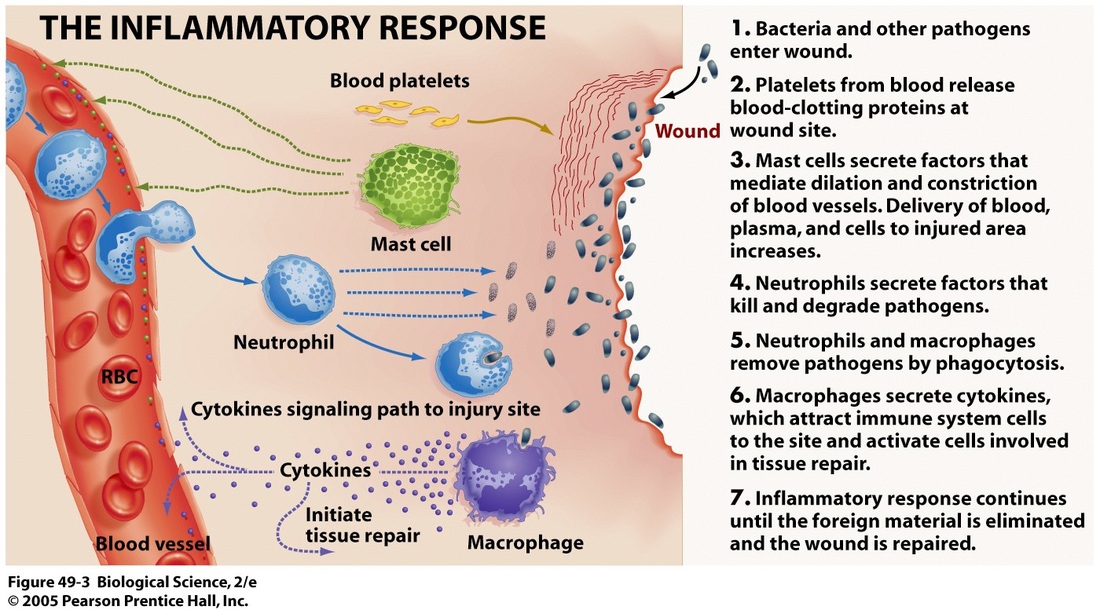
2 types of white blood cell implicate non-specific immune response: neutrophils and macrophages and, unlike in specific response, these cells target any foreign pathogen they detect. Non specific immune response is important as it allows is to protect ourselves against cellular invaders our body has never previously encountered i.e. the common cold (which is forever mutating into a new virus). This response may also trigger a specific response where the action taken by white blood cells is insufficient or they simply detect the foreign body first. When cells become damaged or infected they may either begin attacking he offending bacteria or secrete a hormone called histamine. When cells attack pathogens they present the same antigens on their membrane, which signals to macrophages to "eat" them. The release of histamine may occur in this time as well or instead. The histamine secretions attract neutrophils and increase blood and lymph flow to the affected area causing the dilation of blood vessels and an increase of immunoproteins to the site. Neutrophils and other white blood cells carried over in the excess blood flow bind to pathogens to expand their molecular size; thereby preventing them from re-entering the blood. The now larger molecules may only circulate the body in lymph ducts and so are then transported away from the site of detection to lymphatic organs such as lymph nodes. Where it is necessary, specific response is then initiated in the lymph nodes by anti-presenting cells.